The hotly anticipated Covid-19 vaccines are almost here. Now for the issue of how to dispense them to the masses.
Across the globe, governments are gearing up to roll out nationwide inoculation campaigns, as the development of a handful of experimental vaccines inches closer to the finish line. They are set to face a host of challenges and make many judgment calls in their vaccination strategies.
With several vaccines having proven effective in large clinical trials, regulators may grant approval for their use in the coming weeks, and distribution is set to start immediately afterwards.
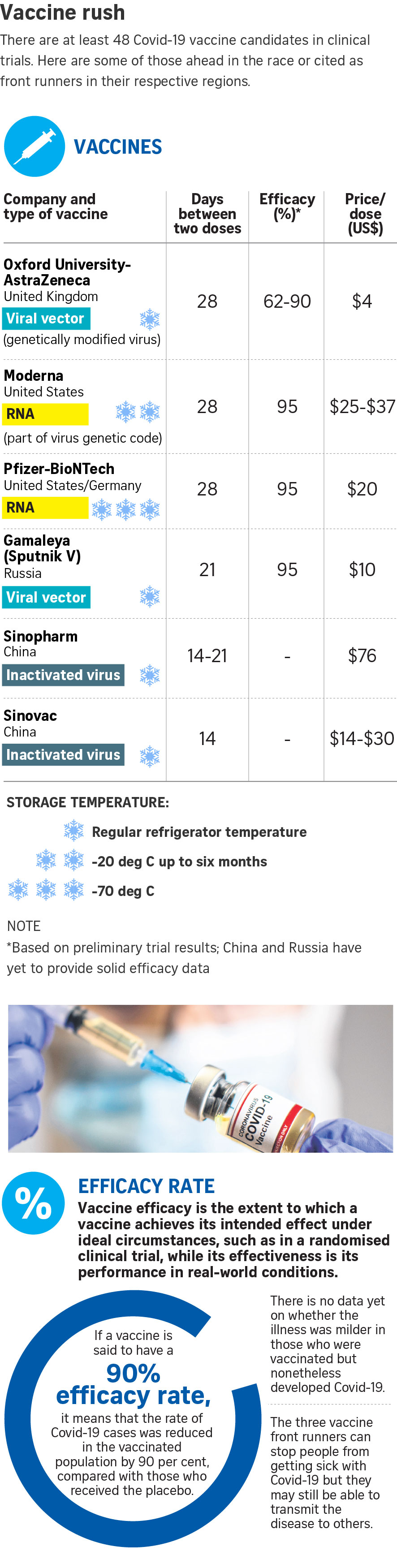
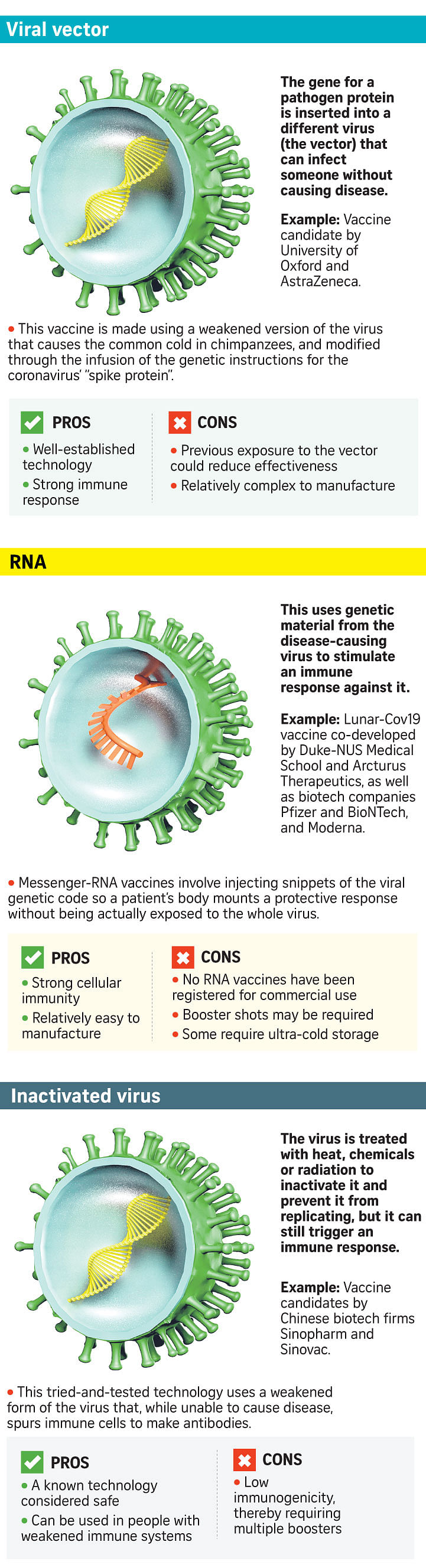
"We need to be able to make a lot of vaccine for the world quickly… (so) diversity is going to be good here," said Professor Sarah Gilbert, a leader of the team working on Britain's Oxford University-AstraZeneca vaccine, in an Associated Press report earlier this week.
Who goes first, and why?
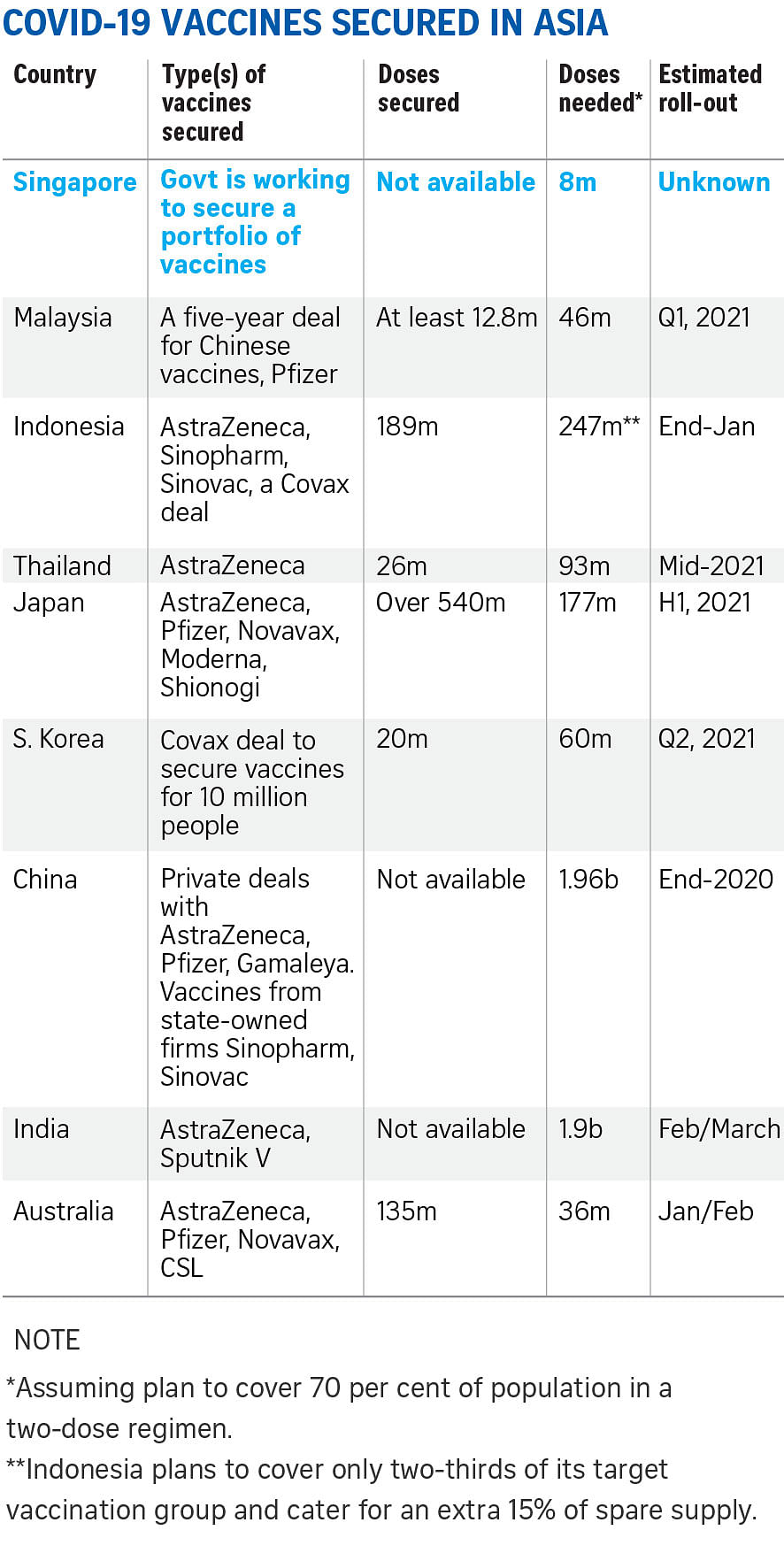
With most of the vaccine front runners involving Western developers, Asian nations are expected to initially receive less of the precious commodity and at later stages than their American and European counterparts.
Richer and more powerful countries, as well as those that helped in testing or producing the vaccines, may also gain access to them sooner.
Upon receiving the vaccines, governments will have to get them into their citizens' arms as soon as possible to bring a swift end to the pandemic. Pertinent issues include who among the populace will be entitled to a spot at the front of the queue. Priorities will differ from country to country.
Malaysia, for one, has said it will focus on inoculating only adults, as the experimental vaccines have yet to be tested on children under the age of 12. The United States-Germany team working on the Pfizer-BioNTech vaccine has only just begun testing on teenagers.
Indonesia intends to cover two-thirds of its people aged 18 to 59 who are deemed fit and without pre-existing health conditions, as most of the vaccine trials have excluded people outside this age bracket. Healthcare and emergency service workers will get the shots before everyone else. The elderly can get vaccinated on a voluntary basis.
Japan, meanwhile, plans to grant its elderly priority over those with chronic diseases, as research shows older people face significantly higher risks of contracting severe Covid-19. The country has the world's largest elderly population, with nearly 29 per cent - more than one in every four people - aged 65 or older.
India is likely to give its healthcare and front-line workers topmost priority as "they are at maximum risk of exposure to the virus", a senior health ministry official said this week.
The strategy makes sense as it is paramount for India - with the world's second-highest number of Covid-19 cases after the United States - to keep its healthcare system up and running to deal with its flood of infections.
Malaysia and India are looking into offering free vaccinations, and Japan has already confirmed it will do so for all its residents. Indonesia is covering vaccinations for 30 per cent of those in its target vaccination group, while the others have to pay for their own shots.
Speed is not a key concern for all, though. South Korea is in no hurry to ink deals despite having been offered more than 30 million doses of vaccines by pharmaceutical firms.
"What's important is to choose the safest and most effective vaccine and to acquire them at an acceptable and reasonable price," Health Minister Park Neung-hoo said last Sunday.
South Korean drugmakers such as SK Bioscience and Celltrion are also developing their own Covid-19 vaccines.
"There's no reason to bear the risk and rush to pre-order vaccines when you can maintain a (comparatively) low number of cases," Dr Chul-woo Rhee, a research scientist at the International Vaccine Institute in Seoul, was quoted as saying in a Wall Street Journal report last week. "South Korea is not in an urgent situation like the US or Europe."
A delicate balance
A recent US study has suggested that prioritising vaccinating seniors aged above 60 would have the biggest impact in lowering Covid-19 deaths, while vaccinating young adults first would have a greater impact on lowering transmission rates. In that light, most countries' vaccination strategies appear aimed first and foremost at preventing deaths.
In Europe, Britain is taking a largely age-based approach, with elderly care home residents and people aged over 80 on top of its list. Staff in care homes and healthcare settings are also prioritised to minimise the risk of transmitting the disease to their charges. Getting inoculated will cost £25 (S$45) for a two-dose regimen.
France's inoculation guidelines include prioritising its five million workers in high-risk jobs, such as shop employees and transport workers with frequent public contact. This came after public consultation to ensure enough people would choose to get vaccinated.
Over in the US, the National Academies of Sciences, Engineering and Medicine has proposed a five-phase plan with healthcare workers and first responders on top of the list, followed by people with high-risk underlying conditions and older adults in densely populated settings.
Experimental shots
In the meantime, large numbers of people in Russia and China have already received experimental vaccine shots.
Russia has administered its Sputnik V vaccine to at least tens of thousands of volunteers outside clinical trials, including medical workers and school teachers.
However, geography teacher Leonid Perlov, 60, told the Washington Post that he declined a vaccination offer as "it has not passed all of the necessary stages of testing".
"The biology teachers are (also) not in a hurry to get vaccinated," Mr Perlov noted of the response among his peers.
"They're more cautious. But the history teachers are the ones ready to volunteer."
In China, about a million people have been inoculated with a vaccine from Sinopharm - one of the country's front runners - despite the state company having yet to show solid late-stage clinical data of its efficacy. Two doses will cost under 1,000 yuan (S$200).
"Among construction personnel, diplomats and overseas students who have travelled to more than 150 countries in the world, there has not been a single case of infection after inoculation," Sinopharm said this month.
Attitudes towards vaccines
Chinese citizens have among the world's highest Covid-19 vaccine acceptance rates, according to an Ipsos survey conducted jointly with the World Economic Forum, which polled more than 18,000 adults from 15 countries last month.
Some 85 per cent of Chinese respondents said they would definitely get inoculated when a Covid-19 vaccine is available.
The poll also showed Indians were the most willing to do so, at 87 per cent, with South Koreans in the third spot at 83 per cent. The French were the most resistant to the idea, at 54 per cent.
Those who said they did not want to receive a coronavirus vaccine were chiefly concerned about side effects - with respondents in Japan and China among those most worried - or that the clinical trials had been too rushed.
To be sure, vaccine makers will need a lot more data on how well their treatments perform in different age and ethnic groups and among people with health conditions, before regulators can give them the nod for public use.
For now, no country has announced plans to make Covid-19 vaccination mandatory.
Some governments have already ruled this out, including France, Britain and Japan, though they emphasised that their citizens would be strongly encouraged to get the shots.
"Mandatory vaccination is rarely justified," said Dr Vageesh Jain from the University College London Institute for Global Health. "The successful roll-out of Covid-19 vaccines will require time, communication and trust."
Other health experts have argued the case for compulsory inoculation for some groups as it could significantly lower the risk of seriously harming or even killing others.
Several airlines and employers are considering ways to implement mandatory vaccination policies.
"The less burdensome it is for an individual to do something that prevents harm to others, and the greater the harm prevented, the stronger the ethical reason for mandating it," said Dr Alberto Giubilini from The Oxford Uehiro Centre for Practical Ethics and author of the book, The Ethics Of Vaccination.
Immunologists agree that countries would have to inoculate around 60 per cent to 70 per cent of their populations to achieve herd immunity against the coronavirus. Exactly how to do so will be a key challenge for governments around the world in the year to come.