Hospitals ramp up battle against bed sores
At CGH, alternating pressure mattresses cut risk for its patients
Sign up now: Get ST's newsletters delivered to your inbox

Patients at Assisi Hospice.
PHOTO: ST FILE
Follow topic:
As Singapore ages, the battle against bed sores in hospitals has taken on a greater urgency.
Experts estimate that at least one in 10 geriatric patients gets bed sores, or pressure ulcers, if they are in hospital for more than a week.
At Changi General Hospital (CGH), about 15 per cent of patients in its geriatric wards used to get bed sores until it set up a task force to combat the problem in April last year. Today, just 4 per cent suffer from this, and those who do are generally diagnosed early and cured.
While all public hospitals have mounted similar efforts, CGH is the only one that provides, for free, an alternating pressure mattress that cut the risk of getting bed sores. Others charge $10 to $20 a day for its use.
Such mattress have little "hills" which move up or down so the pressure on the body changes every few minutes, easing the pressure on the skin, so that sores do not form. This is important as these patients spend many hours prone in bed.
Dr Samuel Chew, a geriatric doctor at CGH, said: "Prevention is the key. The hospital decided it's better to spend money on providing the mattresses than to treat patients for bed sores."
This is because bed sores can form within hours, and often take weeks, months or even years to treat while raising costs and prolonging hospital stays.
Now, about 200 mattresses are in use at any one time, said Advanced Practice Nurse Png Gek Kheng, who heads the CGH task force.
In some British hospitals, as many as one in three elderly patients gets bed sores while in hospital for some other problem - adding about £2 billion (S$4.2 billion) a year to the cost of care.
In the United States, where about 15 per cent of patients get bed sores in hospital, the cost of treating just one sore ranges from US$37,800 (S$53,970) to US$70,000, depending on how bad the sore is, and adds US$11 billion to national healthcare costs.
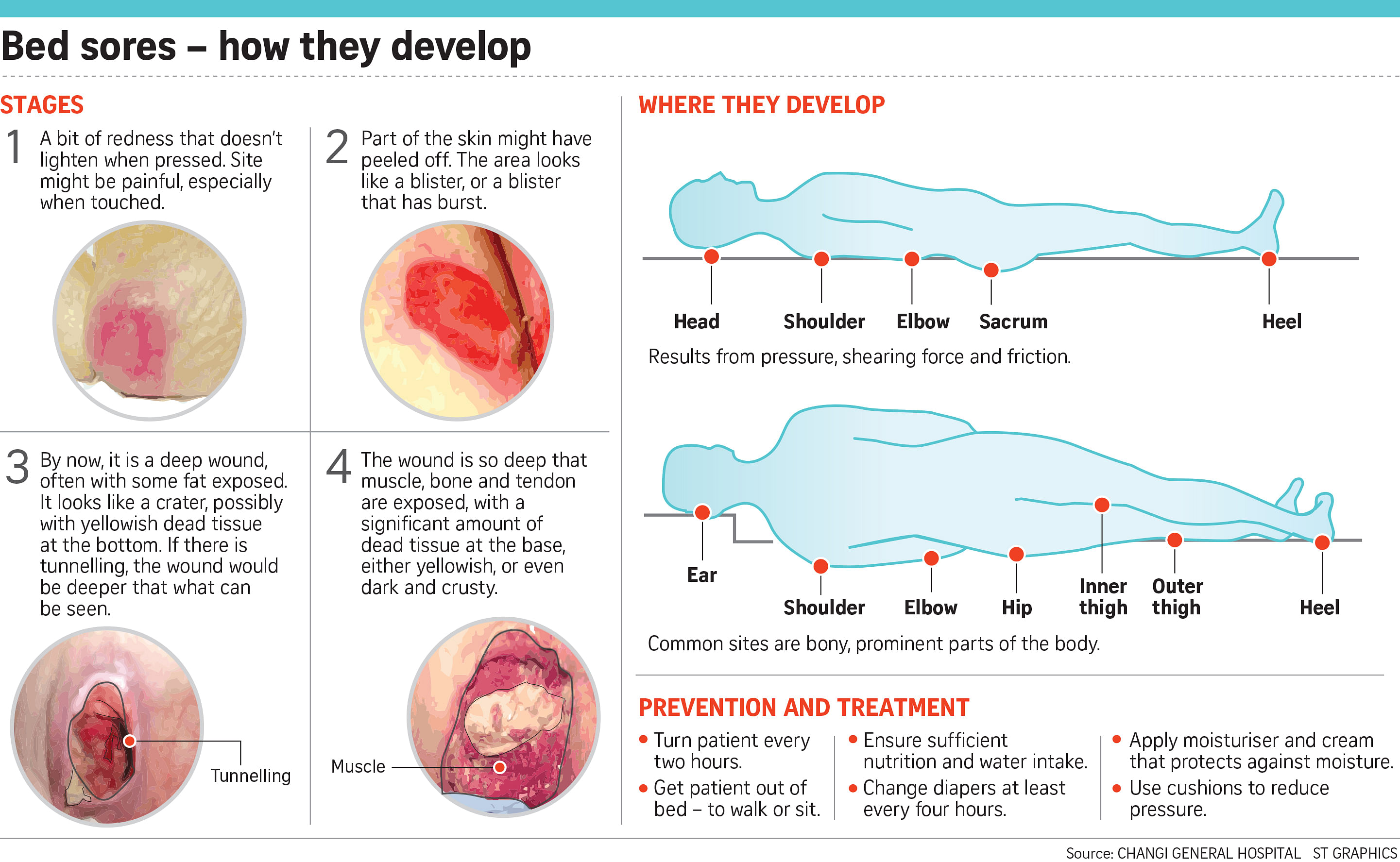
A bed sore starts as a sensitive or painful red patch on the skin, usually near a bony area. Untreated, it can worsen, with the skin flaking off and the flesh underneath rotting. In very bad cases, the wound can be so deep that not just the underlying muscle, but even the bone can be seen.
A major cause of bed sores is constant pressure on an area, especially if it rubs against the bone. Sores can also be caused by friction when a patient is pulled to a different position, or by moisture from wet diapers.
One patient suffered from a severe attack of meningitis 21/2 years ago that had him in hospital intensive care for six weeks.
He is now wheelchair-bound. But that was not his only problem. While in hospital, he developed a bed sore on his buttock.
Now, more than two years later, the sore is still there, although very much better, with the bone no longer exposed. He needs to change the dressing on the wound two to three times a day, as well as go for treatment twice a week at a community hospital . It costs him $50 per visit.
The Agency for Integrated Care subsidises up to 90 per cent of the cost of the mattresses for people in need under the Seniors Mobility and Enabling Fund.
Last year, it helped 1,400 seniors who were "prescribed" such mattresses by nurses or therapists for use at home. Depending on their needs, the mattresses could be simple ones of foam or gel, with prices ranging from $108 to $368.

